Diabetes Emergency Response Guide
Interactive decision tool for hypoglycemia and hyperglycemia reactions
Enter the patient's data to see the recommended emergency protocol.
Note: This is a guide based on the article. Always prioritize emergency services (911) in critical situations.Imagine a situation where a loved one suddenly becomes confused, sweaty, or completely unconscious. If they have diabetes, you aren't just looking at a fainting spell; you're likely facing a medical emergency caused by their medication. Whether it's a dangerous drop in blood sugar (hypoglycemia) or a skyrocketing surge (hyperglycemia), the window to act is small, and the wrong move can be catastrophic. Knowing exactly how to react in these moments doesn't just reduce panic-it saves lives.
Quick Facts for Emergency Response
- Severe Hypoglycemia: Blood glucose below 54 mg/dL (3.0 mmol/L). Requires immediate glucagon or emergency services.
- Severe Hyperglycemia: Blood glucose typically over 250 mg/dL with ketones (DKA) or over 600 mg/dL (HHS). Requires hospital-grade IV fluids and insulin.
- The Golden Rule: Never give food or drink to an unconscious person due to the risk of choking (aspiration).
- Glucagon Speed: Nasal sprays work faster (10-15 mins) than traditional injections (15-20 mins).
Understanding the Danger Zone: Hypoglycemia
When someone on insulin or certain tablets takes too much medication or misses a meal, their blood sugar can crash. Severe Hypoglycemia is a critical state where blood glucose levels drop below 54 mg/dL, often leading to cognitive impairment, seizures, or loss of consciousness. For people with type 1 diabetes, the risk is high, with some facing a 30% annual chance of a severe episode. The primary culprit is usually insulin therapy, though other medications can play a role.
If the person is awake and alert, use the Rule of 15. Give them 15 grams of fast-acting carbs-think four glucose tablets or 4 ounces of regular soda. Wait exactly 15 minutes, check their sugar, and repeat if it's still below 70 mg/dL. However, if they are unconscious or unable to swallow, you must move to emergency medication immediately.
Life-Saving Tools: Modern Glucagon Options
For years, the only way to treat a crash was a cumbersome kit that required mixing a powder and liquid. That has changed. We now have Glucagon, a hormone that triggers the liver to release stored glucose into the bloodstream. Modern versions make this process nearly instant.
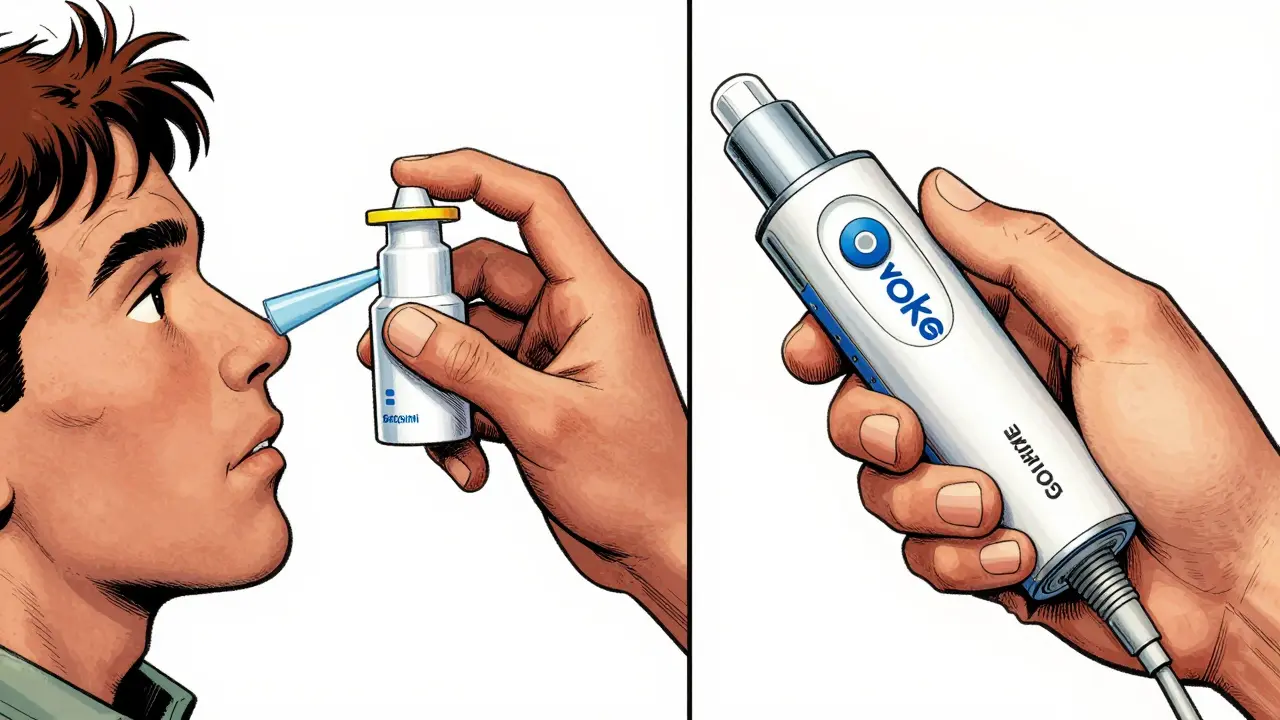
You'll likely encounter three main types of delivery. Baqsimi is a nasal powder that requires no needles-you just spray it up the nose. Gvoke is an autoinjector that works with a simple press-and-hold motion. Then there is the traditional Glucagon Emergency Kit, which is cheaper but much harder to use under pressure. In fact, studies show that while 83% of caregivers can successfully use the nasal spray, only 42% manage the traditional kit correctly. The difference in speed is stark: a nasal dose can be administered in 27 seconds, compared to over two minutes for the old kits.
| Feature | Baqsimi (Nasal) | Gvoke (Autoinjector) | Traditional Kit |
|---|---|---|---|
| Admin Time | ~27 Seconds | Fast | ~2+ Minutes |
| Ease of Use | Very High | High | Low (Requires mixing) |
| Peak Effect | 10-15 Minutes | 15-20 Minutes | 15-20 Minutes |
| Approx. Cost | $268.80 | $259.20 | $130.00 |
The Other Extreme: Hyperglycemic Crises
On the flip side, too little insulin or a severe infection can send blood sugar soaring. This isn't just "high sugar"; it's a systemic failure. Diabetic Ketoacidosis (or DKA) is a life-threatening condition where the body produces excess blood ketones, making the blood acidic (pH below 7.3). This usually happens when glucose is above 250 mg/dL. If left untreated, DKA has a terrifying 70% mortality rate.
Then there is Hyperosmolar Hyperglycemic State (or HHS), a condition seen mostly in type 2 diabetes where glucose levels often exceed 600 mg/dL, causing extreme dehydration. Unlike hypoglycemia, you cannot treat these at home with a quick fix. These are hospital emergencies.
Emergency Care Protocols in the Hospital
When a patient arrives at the ER with severe hyperglycemia, the medical team follows a rigid three-pronged attack. First is fluid replacement. They'll typically pump 1 to 2 liters of 0.9% saline into the veins in the first hour to combat dehydration. Second is electrolyte management. Because insulin shifts potassium into cells, doctors add potassium chloride (20-30 mEq/L) to the IV fluids if serum potassium drops below 5.2 mEq/L. Finally, they use a continuous insulin infusion, starting with a bolus and following with a steady drip of 0.1 units/kg/hour.
A common and dangerous mistake is trying to "fix" hyperglycemia at home by injecting massive doses of insulin without checking for ketones. This can lead to severe hypokalemia (low potassium), which can stop the heart. If blood ketones are over 1.5 mmol/L, the only safe place for the patient is the emergency department.
Preventing the Crisis: A Preparedness Checklist
The scariest part of these emergencies is the 73% of episodes that happen at home where the caregiver is unprepared. To avoid this, every person on insulin needs a strategy. Don't just buy a kit and put it in a drawer; the complexity of old kits means only 5% were ever actually used in a crisis. Practice is the only way to ensure success.
Build your home emergency kit with these specifics:
- Glucose Tablets: Exactly 4g of glucose per tablet.
- Fast Carbs: Pre-portioned 15g servings (juice, honey, or soda).
- Glucagon: A ready-to-use formulation (Baqsimi or Gvoke) with a visible expiration date.
- Monitoring Gear: A reliable glucometer and ketone test strips.
- Contact List: Emergency numbers and the patient's endocrinologist.
Future Outlook and Tech Interventions
We are moving toward a world where the human element of panic is removed. The FDA recently approved the Beta Bionics iLet, a dual-hormone artificial pancreas. Unlike standard pumps, this system can automatically deliver microdoses of glucagon to stop a crash before it happens. While only a few centers currently offer it, this tech could slash severe hypoglycemia mortality by 40% by 2030.
We're also seeing the rise of companion apps, like the Gvoke HelperApp, which guide caregivers through the administration process in real-time. The goal is to close the equity gap; currently, Black and Hispanic patients face significantly higher hospitalization rates due to lack of access to these advanced emergency tools.
What should I do if a diabetic person is unconscious?
Call emergency services immediately. Do NOT try to pour juice or put food in their mouth, as they can choke. If you have a glucagon kit (like Baqsimi or Gvoke), administer it immediately according to the instructions. This is the only safe way to raise their blood sugar without them being awake.
Can I give insulin to someone who is confused and sweaty?
No. Confusion, sweating, and shakiness are classic signs of hypoglycemia (low blood sugar). Giving insulin in this state would lower their sugar even further and could be fatal. If you cannot measure their blood glucose immediately, it is generally safer to treat for hypoglycemia with glucose or glucagon than to risk giving insulin.
How do I know if high blood sugar has become an emergency?
If blood glucose is over 250 mg/dL, you must check for ketones. If blood ketones are above 1.5 mmol/L, or if the person is vomiting and unable to keep fluids down, they are likely entering Diabetic Ketoacidosis (DKA) and need an emergency room immediately.
Is nasal glucagon better than the injection kit?
For most caregivers, yes. Nasal powder (Baqsimi) is significantly faster to administer (under 30 seconds) and removes the need for needles or mixing chemicals. It also tends to raise blood glucose slightly faster than injectable versions.
What is the 'Rule of 15' for mild lows?
The Rule of 15 involves eating 15 grams of fast-acting carbohydrates, waiting 15 minutes, and then re-testing blood glucose. If the level is still below 70 mg/dL, you repeat the process. This prevents "over-treating" and causing a massive blood sugar spike.



Billy Wood on 14 April 2026, AT 01:34 AM
Stay prepared!!! Save lives!!!